In summary, the pathophysiology of ZD is complex and likely to be multifactorial, with contributions from the multiple processes described above.Īaron J. 15 Manometric studies evaluating UES function and pressure have been inconsistent, and it stands to reason that these technical challenges account for the varied results. Furthermore, results are often confounded by the inherent asymmetry of the UES. The process of collecting measurements stimulates the swallowing reflex, resulting in catheter displacement and loss of data. 14 However, the technical difficulties of manometric studies of the UES have proven to be substantial and limiting. found that UES opening was significantly reduced and intrabolus pressures significantly increased in patients with ZD compared to controls. Manometric pressure recordings in patients with ZD have revealed abnormalities of the UES during swallowing. Proposed causal explanations for GERD include persistently elevated CP tone or spasms secondary to reflux, or that acid-induced esophageal shortening results in a gap between the constrictors and the CP, allowing for herniation caudal to the pharyngeal constrictors. 12 Though these studies suggest a possible relationship, no direct causal association has been identified. further supported this association with findings of the presence of Barrett's esophagus, a known complication of GERD, in approximately 15%–20% of ZD patients. found that nearly all of their patients with ZD had GERD. 9 Early studies report an increased incidence of hiatal hernia and GERD in ZD patients. Several authors have noted an association between gastroesophageal reflux disease (GERD) and ZD since the early 1970s. 8 Nevertheless, whether these histological changes are the etiology or the result of ZD is unknown. It is thought that these structural changes are responsible for reduced upper esophageal sphincter (UES) opening during deglutition in ZD patients. noted an increased collagen to elastin ratio in the CP muscle in ZD patients. Histological analysis of CP muscle biopsies from 14 patients with ZD obtained at the time of diverticulectomy to 10 controls obtained via autopsy revealed abundant fibrosis within the CP muscle of ZD patients. suggested CP dysfunction occurs due to muscle fiber degeneration and replacement with fibroadipose tissue. The most widely accepted theory is that incoordination of the IPC muscle with an abnormally functioning CP muscle leads to increased intraluminal pressure, resulting in gradual, progressive mucosal herniation at the site of the inherently weak Killian's triangle. While considerable debate exists with respect to the mechanism of ZD development, a dysfunctional CP muscle is most often implicated. 
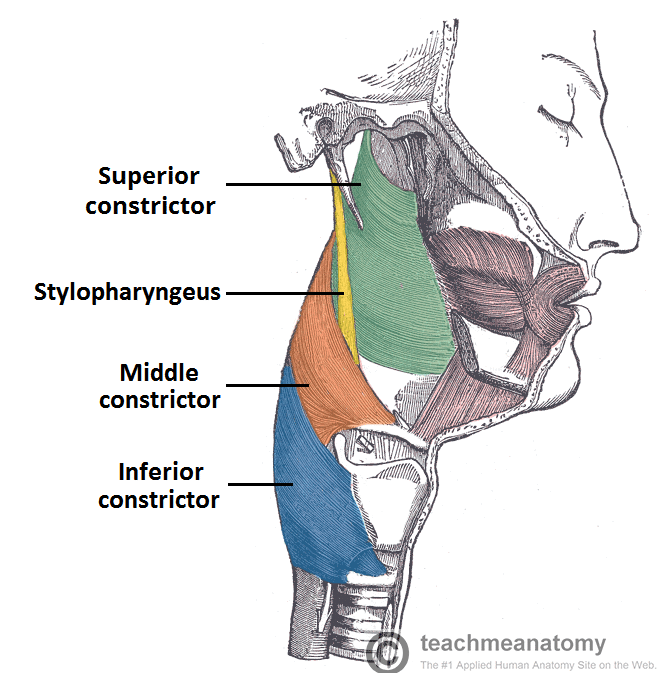
Chhetri MD, in Dysphagia Evaluation and Management in Otolaryngology, 2019 Pathophysiology The muscle is a quadrilateral muscle, thinner and paler than the inferior pharyngeal constrictor muscle and middle pharyngeal constrictor muscle.Nausheen Jamal MD. It is the highest located muscle of the three pharyngeal constrictors. Pharynx Anatomical terms of muscle The superior pharyngeal constrictor muscle is a muscle in the pharynx. Where is the superior pharyngeal constrictor? Do a dry swallow, squeezing all of your swallowing muscles as tightly as you can.Pretend to yawn while holding your tongue back as far as possible.Pretend to gargle while holding your tongue back as far as possible.Inhale and hold your breath very tightly.How do I strengthen my pharyngeal muscles? What is the origin of middle pharyngeal constrictor? Middle pharyngeal constrictor muscle They are innervated by the pharyngeal branch of the Vagus nerve (CN X) with the exception of the stylopharyngeus muscle which is innervated by the glossopharyngeal nerve (CN IX). What nerve Innervates pharyngeal constrictor muscles?ĭuring swallowing, these muscles act to shorten and widen the pharynx. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
